Notes For All Chapters Biology Class 11 CBSE
Excretion is the removal of nitrogenous waste products and other metabolites from the animal body which is normally associated with the process of maintenance of osmibtic concentrations, i.e., osmoregulation within the body.
Both excretion and osmoregulation are important for the maintenance of homeostasis, i.e., for keeping the internal environment of the body constant that is necessary for normal life processes.
Ammonia, urea and uric acid are the major forms of nitrogenous wastes excreted by animals. These substances get accumulated in the animal body either by metabolic activities or by other means like excess ingestion.
Topic 1 Excretion: Major Products, Human System and Uropoiesis
Types of Nitrogenous Excretion
Depending upon the nature of excretory product, animals exhibit different processes of nitrogenous excretion.
These are described as follows
(i) Ammonotelism Ammonia is the most toxic form of nitrogenous waste, it requires large amount of water for its elimination. The organism that excrete ammonia are called ammonotelic and this , process to eliminate ammonia is known as ammonotelism.
Examples of ammonotelic animals are Many bony fishes, aquatic amphibians and aquatic insects. Ammonia, as it is readily soluble, is generally excreted by diffusion across body surfaces or through gill surfaces (in fish) as ammonium ions.
Kidneys does not play any significant role in its removal.
(ii) Ureotelism The process of excreting urea is called ureotelism. Animals, which does not live in high abundance of ‘water convert ammonia produced in the body into urea (in the liver) and release into the blood, which is filtered and excreted out by the kidneys.
Examples of ureotelic animals are Mammals, many terrestrial amphibians and marine fishes.
(iii) Uricotelism The process of excreting uric acid is called uricotelism. Uric acid, being the least toxic nitrogenous waste can be removed with a minimum loss of water from the animal body.
Thus, it is excreted in the form of pellet or paste (i.e., semi-solid form). Normally, the animals which live in desert exhibit uricotelism.
Examples of uricotelic animals are Reptiles, birds, land snails and insects.
Note:
Some animals perform dual excretion, i.e., two modes of excretion. For example, Earthworms excrete ammonia when sufficient water is available, while it excretes urea in drier surroundings.
Other examples are lung fishes, Xenopus, crocodiles, etc.
Excretory Organs
Different animal groups have a variety of excretory structures (organs) to perform the process of excretion. In most of the invertebrates, these structures are simple tubular form, whereas, vertebrates have complex tubular organs called kidneys.
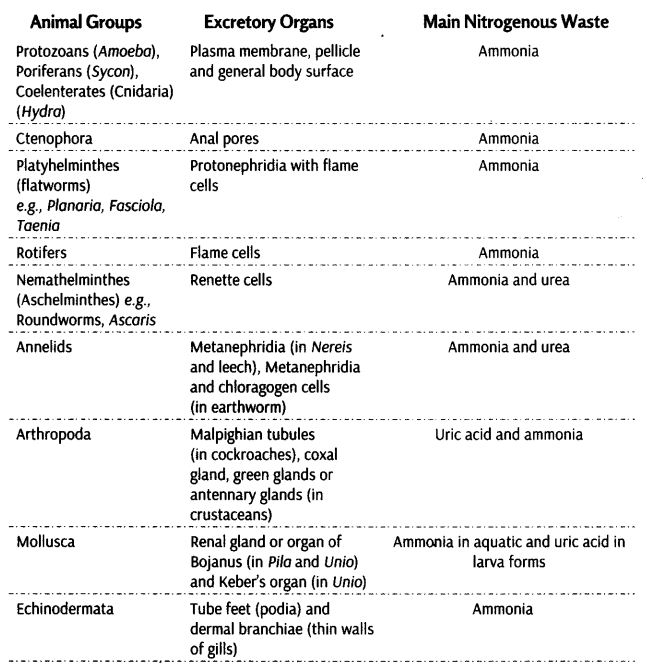
Some of these structures are mentioned below in the given table
Excretory Organs and Main Nitrogenous Wastes of Different Animal Croups
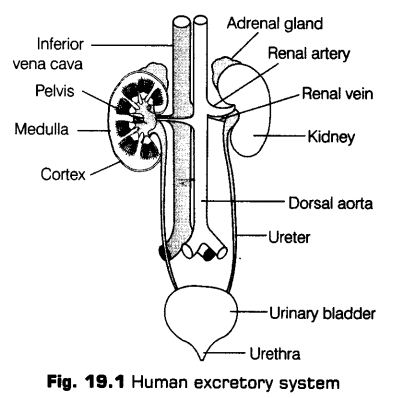
Human Excretory System
Human excretory system consists of a pair of kidneys, a pair of ureters, urinary bladder and urethra, these are described below in detail
1. Kidneys
These are reddish brown, bean-shaped structures situated between the levels of last thoracic and third lumbar vertebra close to the dorsal inner wall of the abdominal cavity. –
Kidneys are mesodermal in origin as they developed from mesodermal nephrostomes or mesomeres (ciliated structures, functional in embryonic conditions).
Position of Kidneys
The kidneys are located below the diaphragm on the left and right sides. The right kidney is lower and smaller than the left kidney because the liver takes up much space of the right side.
Note:
Each kidney of an adult human measures. 10-12 cm in length, 5-7 cm in width, 2-3 cm in thickness with an average weight of 120-170 gm (i.e., 150 gm in males and about 135 gm in females).
Structure of Kidney
Structure of kidney can be studied well under two heads, i.e., external as well as internal structure.
These are described below as
The outer surface of each kidney is convex and inner surface is concave, where it has a notch called hilum, through, which the supply of blood occurs, i.e., renal artery and renal vein, pass in and out of the kidneys along with the ureter and the nerve supply of kidney.
If we look from outside to inside, three layers cover the kidneys, i.e., renal fascia (outermost), the adipose layer and then renal capsule (innermost layer). These coverings protect the kidneys from external shocks and injuries.
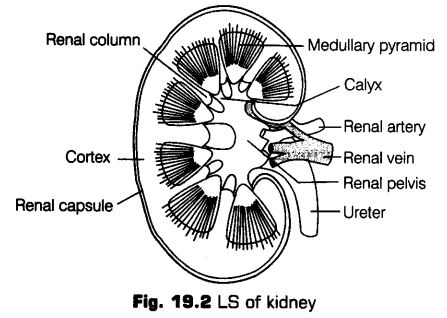
The LS of a mammalian kidney seems to have of an outer cortex and inner medulla.
Inside the kidney, the ureter is expanded as a funnel-shaped cavity called pelvis. The free end of pelvis has number of cup-like cavities called calyces (sing, calyx) major and minor.
Medulla projects into the calyces as conical processes, called renal pyramids or medullary pyramids. The tip of pyramids are called renal papillae. The cortex spreads in between medullary pyramids as renal columns called columns of Bertini.
Microscopic Structure
Each kidney is composed of numerous (nearly one million) complex tubular structure called nephrons, which are the functional units of kidney.
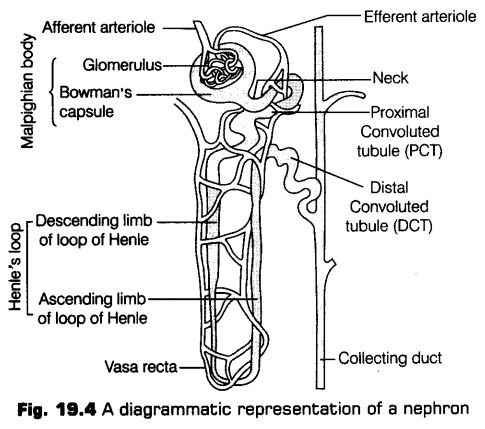
Structure of Nephron Uriniferous Tubule
Each nephron consists of two parts, i.e., the Malpighian body or renal corpuscle and the renal tubule.
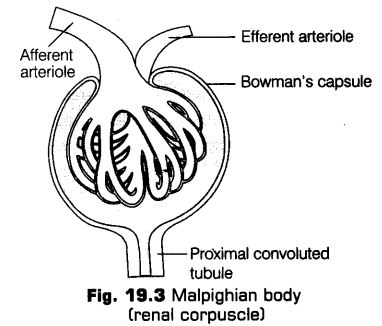
i. Malpighian Body or Renal Corpuscle
Glomerulus along with Bowman’s capsule is called the Malpighian body or renal corpuscle which filters out large solutes from the blood and delivers small solutes to the renal tubule for modification.
* Glomerulus It is a tuft of capillaries formed by the afferent arteriole (a fine branch of renal artery).
The afferent arteriole is short and wide that supplies blood to the glomerulus, while, the efferent arteriole is narrow and long carrying blood away from the glomerulus.
Differences between Afferent Arteriole and Efferent Arteriole
ii. Bowman’s Capsule (Glomerular capsule) It is a double walled cup-like structure that surrounds the glomerulus. The outer parietal wall which is composed of flattened (squamous) cells and the inner visceral wall is composed of a special type of less flattened cells, called podocytes.
iii. Renal Tubules
Just below the glomerulus, the tubule has a very short neck.
Attached to each Bowman’s capsule is a long, thin tubule with three distinct regions.
These regions are described as follows
(a) Proximal Convoluted Tubule (PCT) Behind the neck, it makes few coils and is restricted to the cortical region of the kidney.
(b) Henle’s Loop It is quite narrower and U-shaped (or hair pin-shaped) having a descending limb that ends into the medulla and an ascending limb that extends back from the medulla into the cortex.
Differences between Descending Limb and Ascending Limb of Henle’s Loop
Note:
* Peritubular Capillary Network (PTCN), is formed when a minute vessel of peritubular capillaries runs parallel to the loop of Henle forming a U-shaped vasa recta.
* All these capillaries join to form renal venules, which join to form a renal vein that opens into the inferior vena cava.
Types of Nephrons
Based on the location in the kidney, nephrons are of following two types
1. Cortical Nephrons
In majority of nephrons, the loop of Henle is too short and extends only very little into the medulla i.e., lie in the renal cortex. Such two nephrons are called cortical nephrons.
Juxtamedullary Nephrons
In some of the nephrons, the loop of Henle is very long and runs deep into the medulla. These nephrons are called juxtamedullary nephrons.
The cortical nephron forms about 80% of the total nephron count while rest 20% are the juxtamedullary nephron.
Functions of Kidney
Following functions are served by kidney
(i) Regulation of water and electrolyte balance.
(ii) Regulation of arterial pressure.
(iii) Excretion of metabolic waste and foreign chemicals.
(iv) Secretion of hormones like renin.
2. Ureters
The pelvis of each kidney is continued as a ureter and emerges out at hilus. Ureter is a long and muscular tube. Ureters of both sides extend posteriorly and open into the urinary bladder.
3. Urinary Bladder
It is a thin-walled, pear-shaped, white transparent sac present in the pelvic cavity. It temporarily stores the urine.
4. Urethra
It is a membranous tube, which conduct urine to the exterior. The urethral sphincters keep the urethra closed except during voiding of urine.
The formation of urine is the result of the following processes
1. Glomerular Filtration
The first step of urine formation is the filtration of blood, which is carried out by the glomerulus. That’s why this step is called glomerular filtration.
Kidneys filter about 1100-1200 mL of blood per minute, which constitute roughly l/5th of the blood pumped out by each ventricle of the heart in a minute.
The glomerular capillary bloodpressure causes filtration of blood through three layers, i.e.,
(i) the endothelium of glomerular blood vessels.
(ii) the epithelium of Bowmans capsule.
(iii) a basement membrane (present between the above mentioned two layers).
The podocytes (epithelial cells of Bowman’s capsule) are arranged in such a manner so, as to leave some minute spaces called filtration slits or slit pores.
On account of the high pressure in the glomerular capillaries, the substances are filtered through these pores into the lumen of the Bowman’s capsule (but the RBC, WBC and plasma proteins having high molecular weight are unable to pass out).
That’s why this process of filtration through glomerular capillaries in the Bowman’s capsule is known as ultra filtration and the filtrate is called glomerular filtrate or primary urine.
It is hypotonic to urine that is actually excreted. Basic function of nephron is to clear out the plasma from unwanted substrates and also maintain the osmotic concentration of the blood plasma. Thus, the fluid coming out is known as urine, whose formation occurs inside the kidney.
Glomerular Filtration Rate The amount of the filtrate formed by the kidneys per minute is called Glomerular Filtration Rate (GFR). In a healthy person it was found approximately 125 mL/min, i.e., 180 L/day.
GFR is regulated by one of the efficient mechanism carried out by Juxtaglomerular Apparatus (JGA).
JGA is a special sensitive region formed by cellular modifications in the distal convoluted tubule and the afferent arteriole at the location of their contact.
This apparatus includes
(i) granular juxtaglomerular cells in the afferent arteriole.
(ii) macula densa cells of DCT.
(iii) agranular lacis cells situated in between the above two.
A fall in GFR can activate the JG cells to release renin, which can stimulate the glomerular blood flow and thereby, the GFR back to I normal.
2. Selective Reabsorption
This is the second step in the formation of urine from filtrate. The urine released is 1.5 L as compared to the volume of the filtrate formed per day (180 L). It suggests that as much as 99% of the material in the filtrate is reabsorbed by the renal tubules. Thus, the process is called reabsorption.
Depending upon the types of molecules being reabsorbed, movements into and out of epithelial cells in different segments of nephron occur either by passive transport or active transport.
These are described as follows
(i) Water and urea, are reabsorbed by passive transport (i.e., water is reabsorbed by osmosis and urea by simple diffusion).
(ii) Glucose and amino acids are reabsorbed by active transport.
(iii) The reabsorption of Na+, occurs both by passive and active transport.
3. Tubular Secretion
It is also an important step in urine formation. Certain chemicals in the blood that are not removed by filtration from the glomerular capillaries are removed by this process of tubular secretion. It helps in the maintenance of ionic and acid-base balance of body fluids by removing chemicals like foreign bodies, ions (K+, H+, NH–) and molecules (medicines), etc., that are toxic at elevated levels.
Difference between the Tubular Reabsorption and Tubular Secretion
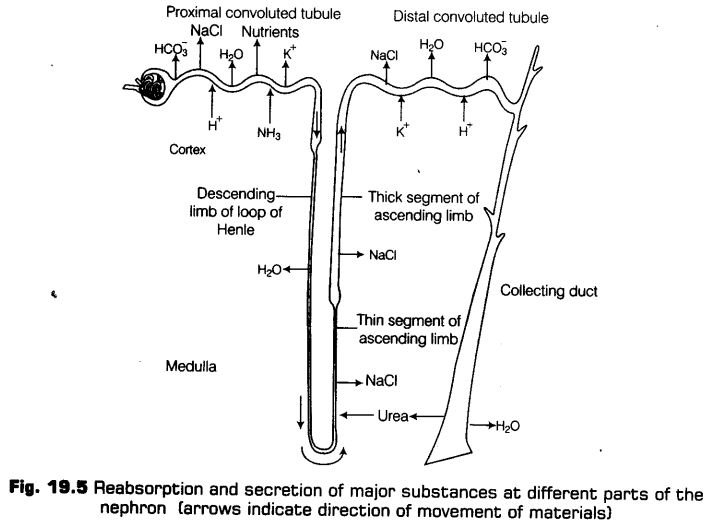
Functions of the Tubules
When the glomerular filtrate/primary urine passes through renal tubule, water and different materials of filtrate reabsorb at various places.
These are given below in the following manner
i. Proximal Convoluted Tubule (PCT)
The epithelial cells of the PCT have numerous microvilli (simple cuboidal brush-border epithelium) which increase the surface area available for reabsorption.
The process of reabsorption mostly (65%) takes place within PCT (i.e., nearly all of the essential nutrients, 70-80% of electrolytes and water). PCT also helps in the absorption of HCO– from the filtrate.
Selective secretion of hydrogen ions, ammonia and potassium ions takes place here to maintain the pH and ionic balance of the body fluids. The filtrate is considered isotonic to blood plasma.
ii. Henle’s Loop
Reabsorption in Henle’s loop is minimum, besides it, this plays an important role in maintaining the high osmolarity of medullary interstitial fluid. Two portions of Henle’s loop, play different role in osmoregulation such as
a. Descending Limb of Loop of Menu?
Water is reabsorbed here due to increasing osmolarity of interstitial fluid but, sodium and other electrolytes are not reabsorbed here. This concentrates the filtrate as it moves down.
b. Ascending Limb of Loop of Menu?
This segment is impermeable to water but permeable to K+,Cl– and Na+ and partially permeable to urea. Thus, in the thick ascending limb of the loop of Henle Na+, K+, Mg2+ and Cl– are reabsorbed.
Therefore, as the concentrated filtrate pass upward, it gets diluted due to the passage of electrolytes to the medullary fluid.
iii. Distal Convoluted Tubule (DCT)
Active reabsorption of sodium ions from the filtrate (under the influence of aldosterone) takes place. Water is also reabsorbed here under the influence of Antidiuretic Hormone (ADH).
With associated secretion of potassium (K+), hydrogen (H+) ions, NH–, some Cl– (chloride) ions and HCO– are also reabsorbed here. It is necessary to maintain the pH and sodium-potassium balance in blood. This makes the filtrate isotonic to blood plasma.
Collecting Duct
This duct extends from the cortex of the kidney to the inner parts of the medulla and is highly permeable to water. Thus, a considerable amount of water is reabsorbed here under the influence of ADH to produce concentrated filtrate. Sodium is also reabsorbed here under the influence of aldosterone.
CT (Collecting Tubule) allows passage of small amounts of urea into the medullary interstitium to maintain the osmolarity. It also plays an important role in the maintenance of pH and ionic balance of blood by the selective secretion of H+ and K+ ions.
Therefore, the filtrate is now called urine. Thus, urine is isotonic to medullary fluid and hypertonic to blood.
Concentrations of important ions and other substances in the blood are controlled by regulating water levels.
Topic 2 Excretion : Various Controlling Mechanisms and Disorders
Counter Current Mechanism
Kidney of higher vertebrates (such as mammals, birds including man) has the ability of absorbing more and more water from tubular filtrate (in the Henle’s loop region) to make the urine more concentrated.
This can be achieved by a special mechanism known as counter current mechanism and also known as urine concentration mechanism.
Basic Concept
(i) Henles loop and vasa recta (capillary loop) play an important role in this mechanism. The flow of filtrate in the limbs of Henle’s loop is in opposite directions and thus, forms a counter current. The flow of blood with in the two limbs of vasa recta also occur in the counter current pattern.
(ii) The osmolarity (i.e., number of Osmols of solute per litre) of renal cortical interstitium is the same (300 m Osmol/ L) as in other tissues, but that of the interstitium of renal medulla is hypertonic with a gradient of hyperosmolarity from renal cortex to the tips of medullary papillae.
The hyperosmolarity of medullary interstitium near the tips of the papillae is as high as 1200-1450 m Osmol/L.
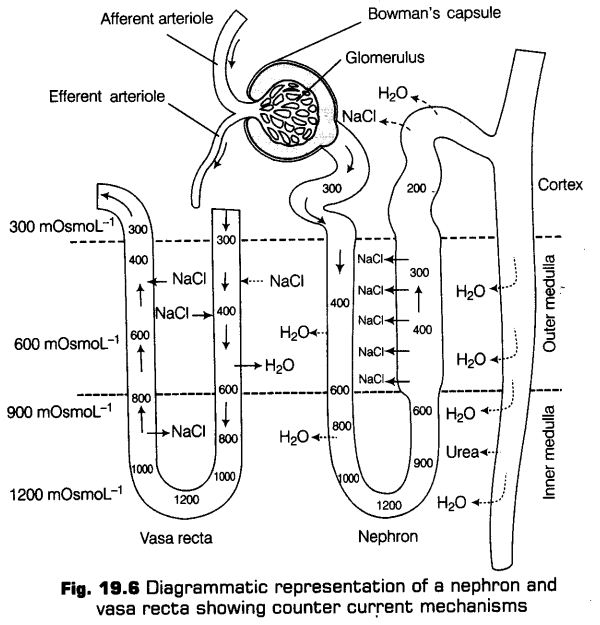
The Mechanism
The gradient of increasing hyperosmolarity of medullary interstitium is maintained by a counter current mechanism and the proximity between the Henle’s loop and vasa recta.
This gradient is mainly caused by NaCl and urea. The transport of these substances is facilitated by the special arrangement of Henle’s loop and vasa recta.
There are two aspect of this mechanism
(i) Counter current multiplication (by the Henle’s loop).
(ii) Counter current exchange (by the vasa recta).
NaCl is transported by the ascending limb of Henle’s loop, which is exchanged with the descending limb of vasa recta.
NaCl is returned to the medullary interstitium by the ascending part of vasa recta. But, contrarily, the water diffuses into the blood of ascending limb of vasa recta and is carried away into the general.blood circulation.
Permeability to urea is found only in the deeper parts of thin ascending limb of Henle’s loops and collecting ducts.
Urea diffuses out of the collecting ducts and enters into the thin ascending limb. A certain amount of urea recycled in this way is trapped in medullary interstitium by the collecting tubule. Thus, collecting tubule also play a minor role in the process (as shown in the figure above).
Note:
The counter current mechanism helps in the maintenance of a concentration gradient in the medullary interstitium.
Presence of such gradient helps in an easy passage of water from the collecting tubule resulting in the formation of concentrated urine (filtrate), i.e., nearly four times concentrated than the initial filtrate formed.
Regulation of Kidney Functions
To maintain homeostasis, the regulation of water and solute contents of the body fluids is performed by the kidneys. The vertebrate kidney is very flexible in its functioning. It excretes larger quantities of dilute urine when water is abundant in the body tissues and small amounts of concentrated urine when there is shortage of water.
Hormones acts as an important signalling molecules in controlling the regulatory processes in the kidneys. The functioning of the kidneys is efficiency monitored and regulated by hormonal feedback mechanisms involving hypothalamus, JGA (Juxtaglomerular Apparatus) and to a certain extent, the heart.
Regulation of the functioning of kidneys can be discussed under the following headings
Regulation by the Hypothalamus
Excessive loss of fluid from the body activates osmoreceptors, which stimulate the hypothalamus to release ADH or vasopressin form the neurohypophysis. ADH facilitates water reabsorption from posterior parts of tubule. An increase in body fluid volume can switch off the osmoreceptors and suppresses the ADH release to complete the feed back. ADH also causes constrictory effects on blood vessels.
This causes an increase in blood pressure, which in turn increase the glomerular blood flow and thereby the GFR (Glomerular Filtration Rate).
Regulation by the Juxtaglomerular Apparatus (JGA)
As blood pressure/glomerular blood flow /GFR decreases, the cells of the JGA release the enzyme renin.
Renin converts angiotensinogen in blood to Angiotensin I and Angiotensin II (active form). This mechanism is generally known as the Renin-angiotensin mechanism.
Angiotensin has following effects
(a) Raises blood pressure by constricting blood vessels (being a powerful vasaconstrictor) and thereby, GFR.
(b) Activates the adrenal cortex to release aldosterone.
(c) Aldosterone causes reabsorption of Na+ and water from the distal parts of the tubule. This also leads
to an increase in blood pressure and GFR.
Regulation by the Heart
Atrial Natriuretic Factor (ANF) produced by the atria of heart can cause vasodilation (dilation of blood vessels) and thereby, decrease the blood pressure.
ANF inhibits NaCl reabsorption and concentration of urine.
Micturition
Urine is produced and drained continuously by the nephron into the renal pelvis from here, it is carried down to the ureters and then into the urinary bladder.
The bladder serves to store the urine temporarily till a voluntary signal is given by the Central Nervous System (CNS). As urine collects, the muscular walls of the bladder distend to accommodate it. .
The stretch receptors on the walls of the bladder set up reflexes (send signals to the (CNS) by stimulating the sensory nerve ending in the bladder). It causes an urge to pass out urine.
The act of expulsion of urine involves the coordinated contraction (as CNS passes on motor messages) of the smooth muscle of the bladder wall and simultaneous relaxation of the internal and external urethral sphincters. The process of release of urine is called micturition and the neural mechanism causing it is called the micturition reflex.
Note:
Alcohol inhibits the release of ADH and caffeine interferes with ADH action and sodium reabsorption. Thus, both of these artificially dilute the urine and are called diuretics. Urination is a reflex response in babies, but is controlled consciously in older children and adults.
Urine
An adult man normally passes about 1-1.5 L of urine per day.
Composition Urine normally contains, water 95%, salts 2%, urea 2.6%, uric acid 0.3%, traces of creatinine, creatine, ammonia, etc.
Colour Pale yellow, due to pigment urochrome produced by the breakdown of haemoglobin.
pH Ranges from 4.5-8.2, average pH 6.0 (i.e., slightly acidic).
Odour Unpleasant, if allowed to stand imparts strong smell like, ammonia.
Note:
Least concentration of urea is found in renal vein because urea is excreted through urine formed in kidney. On an average, 25-30 g of urea is excreted out per day. Highest concentration of urine is found in hepatic vein because urea is synthesised in liver.
Analysis of urine helps in clinical diagnosis of many metabolic disorders as well as malfunctioning of the kidney.
For example, presence of glucose (glycosuria) and ketone bodies (ketonuria) in urine are indicative of diabetes mellitus and presence of protein, blood and pus in the urine is called proteinuria, haematuria and pyuria respectively.
Role of Other Organs in Excretion
Other than the kidneys, there are some accessory excretory organs also that help in the elimination of excretory wastes.
These are described as follows
1. Lungs
Carbon dioxide and water are the waste products formed in respiration. Lungs remove the CO2 and some water as vapour in the expired air. About 18 L of CO2 per hour and 400 mL of water per day are eliminated by human lungs.
2. Liver
It changes the decomposed haemoglobin of the worn-out red blood corpuscles into bile pigments, i.e., bilirubin and biliverdin. These pigments passes into the alimentary canal with the bile for elimination in the faeces. The liver also excretes cholesterol, steroid hormones, certain vitamins and drugs via bile.
Liver deaminates the excess and unwanted amino acids, producing ammonia, which is quickly combined with CO2 to form urea in urea cycle or Ornithine cycle, which is further removed by the kidneys.
3. Skin
The sweat and sebaceous glands in the skin can eliminate certain substances through their secretions.
(i) Sweat Glands The secretion of sweat glands (sweat) is an aqueous fluid containing NaCl, lactic acid, small amounts of urea, amino acids and glucose. Control of sweat lost is an example of homeostasis control, for regulating the body temperature (i.e., to facilitate a cooling effect on the body surface).
(ii) Sebaceous Glands Sebum from sebaceous glands eliminates sterols, fatty acids, waxes and hydrocarbons. This secretion is mainly meant for protective oily covering of the skin.
4. Intestine
Epithelial cells of colon excrete excess salts of calcium, magnesium and iron along with faeces.
5. Salivary Glands
Heavy metals and drugs are excreted in the saliva.
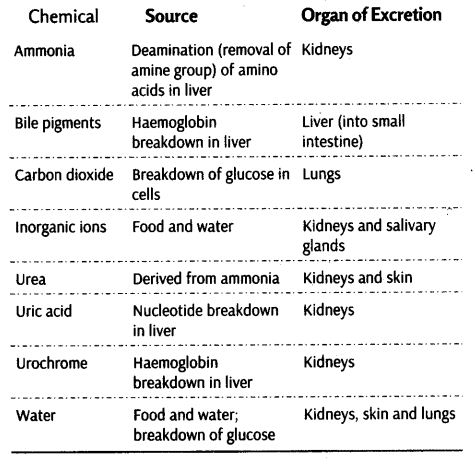
Important Metabolic Wastes and Substances Excreted from the Body
Disorders of the Excretory System
Malfunctioning of kidneys can lead to several disorders of the excretory system.
Some of these are as follows
(i) Uremia It is the presence of an excessive amount of urea in the blood. Urea is highly harmful as it poisons the cells at high concentration and may lead to kidney failure.
(ii) Kidney Failure (renal failure) Partial or total inability of kidneys to carry on excretory and salt-water regulatory functions is called renal or kidney failure.
(iii) Renal Calculi It is the formation of stone or insoluble mass of crystallised salts (calcium, magnesium, phosphates and oxalates etc.), formed within the kidney.
(iv) Glomerulonephritis It is the inflammation of glomeruli of kidney.
Artificial kidney (haemodialyser) is a machine that is used to filter the blood (to remove urea and other nitrogenous wastes) of a person, whose kidneys are damaged.
The process is called haemodialysis.
The outline details of apparatus and the process are as follow
(i) It works on the principle of dialysis (i.e., diffusion of small solute molecules through a semipermeable membrane (cellophane).
(ii) Blood of the patient is pumped from one of the arteries into the dialysing unit (haemodialyser) after cooling it to 0°C and mixing with an anticoagulant (heparin).
(iii) Haemodialyser is a cellophane tube suspended in a dialysing fluid (salt-water solution) of the same composition as that of plasma except the nitrogenous wastes (urea).
(iv) Pores of the cellophane tube allow the passage of molecules based on concentration gradient. Nitrogenous wastes like urea, uric acid, creatinine,excess salts and excess H+ ions easily get diffuse from the blood into the surrounding solution. Thus, the blood is cleared of nitrogenous waste products without loosing plasma proteins.
(v) The blood thus, purified, is warmed to body temperature, checked to ensure that it is isotopic to the patients blood. Now, the blood is mixed with an anti-heparin to restore its normal clotting power and then pumped back to the body of patient through a vein, usually the radial vein.
Kidney (Rena!) Transplantation
Grafting a kidney from a compatible donor to restore kidney functions in a recipient suffering from kidney failure is called renal or kidney transplantation. It is an ultimate method in the correction of acute renal failures.
A living donor can be used in a kidney transplant. It may be an identical twin, a sibling or a close relative to minimize the chances of rejection by the immune system of the host. To prevent the rejection of transplanted kidney, special drugs are also used, which suppress the recipients immune system.




Leave a Reply